We do not diagnose disease or recommend a dietary supplement for the treatment of disease. You should share this information with your physician who can determine what nutrition, disease and injury treatment regimen is best for you. You can search this site or the web for topics of interest that I may have written (use Dr Simone and topic).
“We provide truthful information without emotion or influence from the medical establishment, pharmaceutical industry, national organizations, special interest groups or government agencies.” Charles B Simone, M.MS., M.D.
INFLAMMATION NOT LDL
https://bit.ly/3bPVFsD
Lawrenceville, NJ (Dr Simone) – I have long maintained that it is not the level of cholesterol that increases the risk for cardiovascular disease, cancer, other chronic illnesses and poor athletic performance, but rather it is the inflammation and oxidation from those cholesterol containing foods.
At a medical conference I asked a Chairman of Medicine of a prestigious university how he would treat a man who had a massive heart attack with a cholesterol of only 140, LDL of 50, normal coronary arteries, and no other risk factors. He said ‘That’s a no brainer – give him a high dose statin.’ I then said, “That man’s cholesterol, LDL and coronary arteries are excellent. It’s probably only inflammation or a clot, so one could use vitamins and other nutrients instead.” He abruptly and arrogantly said ‘No, give him a statin’ and he turned away. This is what Big Pharma does. They pay so-called “thought leaders” to influence other doctors to prescribe their drugs. And these “thought leaders” must not deviate from the written words given to them by Big Pharma.
You can see how much any doctor or hospital are paid by Big Pharma on Pro-Publica, an investigative reporting group. You will be surprised at the amount paid by Big Pharma to some doctors and to some major hospitals
https://projects.propublica.org/docdollars/
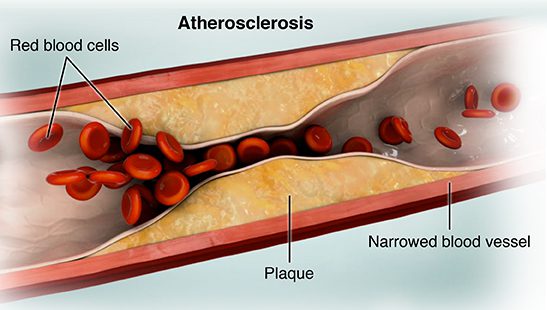
Arteries are composed of living cells. Inflammation initiates the artery lesion by making the adhesion molecule VCAM-1. This attracts white blood cells called monocytes and T-cells that engulf lipids, thus forming the fatty streak progressing to plaque. Narrowing arteries do not necessarily cause a heart attack and treating those narrowed arteries with stents or bypass surgery does not prolong life.
There are multiple lines of evidence that inflammation increases the risk for cardiovascular disease, cancer and other chronic illnesses:
1) I have written that the LDL cholesterol contributed only modestly to overall risk because people who had the most reduction in inflammation, not LDL, had the least recurrent vascular events (information from Lancet August 2014). And that’s why a committee of a mere 15 people changed the US guidelines from treating to a specific LDL target to arbitrarily and capriciously treating patients who were “at high risk” with high dose statin.
DO YOU KNOW YOUR LDL? HDL? TRIGLYCERIDES? ARE THEY IMPORTANT?
2) Genetics of LDL. Is the benefit of statin therapy from lowering lipids or decreasing inflammation? The genetic loci that relate to statin induced LDL reductions are distinct from the genetic loci that are associated with statin induced reductions of inflammation. People who had the most reduction in inflammation had the least recurrent vascular events. People who had low LDL and ordinarily would not require statin treatment but who were treated with statins anyway, had reduced heart attacks, strokes, and all-cause mortality.
3) Another line of evidence shows that lowering LDL to very low levels using an antibody (evolocumab) did not extend life and in fact there were more deaths in the treatment group.
LOW LDL DOES NOT PROTECT, BUT BIG PHARMA AND HARVARD SAY YES
4) CANTOS Trial – patients were given a monoclonal antibody (canakinumab) to lower a protein in their bodies that causes inflammation, interleukin-1Beta. This antibody reduced inflammation and reduced cardiovascular events, including stroke, without lowering cholesterol or LDL-cholesterol (1). The patients taking this antibody had a higher incidence of fatal infection and there was no significant difference in mortality. In addition, the prohibitive cost is $200,000 a year. The conclusion though is important: Decreasing inflammation will decrease risk of cardiovascular events without lowering cholesterol or LDL-cholesterol. In addition, those patients who received the highest dose of this antibody had a 51% lower cancer mortality and a 77% lower lung mortality (2).
(5) Other inflammatory diseases like rheumatoid arthritis, psoriasis, and inflammatory bowel disease have a high risk for cardiovascular disease. Those patients receive antiinflammatory treatments and have a decrease risk of cardiovascular disease and cardiovascular events (3,4).
(6) CIRT Trial – Methotrexate, a non-specific antiinflammatory medicine did not reduce C-reactive protein and did not result in fewer cardiovascular events than placebo. This trial did not screen for C-reactive protein level but instead required participants to have either diabetes or the metabolic syndrome. Authors write “It is thus possible that the ability of methotrexate to reduce the C-reactive protein level is limited to clinical situations in which inflammation levels are high.” https://www.nejm.org/doi/full/10.1056/NEJMoa1809798
(7) COLCHICINE Cardiovascular Outcomes Trial (COLCOT) – a randomized double blind study involving 4745 patients using colchicine that is usually used to treat inflammatory conditions like gout and pericarditis. “Among patients with a recent myocardial infarction, colchicine at a dose of 0.5 mg daily led to a significantly lower risk of ischemic cardiovascular events than placebo.” https://www.nejm.org/doi/full/10.1056/NEJMoa1912388
(8) COLCHICINE at .5 mg daily in a randomized trial of 5522 patients significantly decreased the risk of cardiovascular events in patients who already have chronic coronary disease. NEJM. 2020; 383:1838-47. https://www.nejm.org/doi/full/10.1056/NEJMoa2021372
Lowering LDL-C using statins had an inconsistent impact on heart attack, stroke, all-cause mortality. Change the “guidelines” to reflect this finding.
https://jamanetwork.com/journals/jamainternalmedicine/article-abstract/2790055
“We conclude that the expectation that Cardiovascular Heart Disease could be prevented or eliminated by simply reducing cholesterol appears unfounded.”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4513492/
In fact, multiple studies show that statins can cause atherosclerosis. “Thus, the promotion of statin treatment by the Consensus Statement from the European Atherosclerosis Society Consensus Panel 2017 is rather risky and we do not feel that the conclusions are justified for the prevention of ASCVD.”
https://pubmed.ncbi.nlm.nih.gov/29353277/
Dr Simone’s Recommendation
People take statins, their blood values look great, they are happy and their doctors are happy, but they continue eating inflammatory foods. Follow our SIMONE TEN POINT PLAN.
http://drsimone.com/tenpoint.htm
IT’S ALL ABOUT INFLAMMATION AND OXIDATION. Lipids are markers of foods that increase inflammation and oxidation. So if you take prescription medications or nutrients to lower your lipids but continue eating high fat, high sugar, low fiber foods, you will continue to cause inflammation and oxidation in your body. Other controllable risk factors like overweight / obesity, smoking, alcohol, etc, also increase inflammation and oxidation.

INFLAMMATION AND OXIDATION – WHAT YOU CAN DO
You should consider taking antioxidants in the correct doses, correct chemical forms, and correct ratios of one to another. Also take anti-inflammatory agents.
Anti-Inflammatory Foods
-
Green leafy veggies such as spinach, kale, and collards.
-
Fruits and vegetables that have color like blueberries, pineapples, strawberries, cherries, and oranges. Quercetin is found in these and is an antioxidant and anti-inflammatory agent.
-
Walnuts and fatty fish have high amounts of omega 3 fatty acids: wild-caught salmon, mackerel, tuna, and sardines.
Supplements to reduce inflammation
-
Alpha-Lipoic Acid
-
Curcumin is a component of the spice Turmeric.
-
Omega 3 fatty acids
-
Ginger
-
Resveratrol
-
Cayenne
-
Cinnamon
-
Cloves
-
Sage
-
Rosemary